Exercise and Type 1 Diabetes
The following are general recommendations from the American Diabetes Association and the Juvenile Diabetes Research Foundation. We encourage you to follow your own personalized diabetes plan, and speak with your endocrinologist about concerns or making any changes to your care plan.
With type 1 diabetes, it’s very important to balance your insulin doses with the food you eat and the activity that you do—even when you are doing house or yard work. Planning ahead and knowing how your blood sugar and body respond to exercise can help you keep your blood sugar from going too low or too high. Before you begin exercise, it is first important to make sure your blood sugar is in safe range.
Preventing lows
Sometimes people experience a drop in blood sugar during or after exercise, so it is very important to check your blood sugar, plan ahead, and be prepared to treat hypoglycemia (low blood sugar).
There are a few ways that exercise lowers blood sugar:
- Insulin sensitivity is increased, so your muscle cells are better able to use any available insulin to take up glucose during and after activity.
- When your muscles contract during activity, your cells are able to take up glucose and use it for energy whether insulin is available or not.
Physical activity can lower your blood sugar up to 24 hours or more after your workout by making your body more sensitive to insulin.
Your blood sugar response to exercise will vary depending on:
- Blood sugar prior to beginning exercise
- Intensity of exercise
- Low long you are active
- Any changes you’ve made to insulin dosages
Become familiar with how your blood sugar responds to exercise. Checking your blood sugar level more often before and after exercise can help you see the benefits of activity. You also can use the results of your blood sugar checks to see how your body reacts to different activities. Understanding these patterns can help you prevent your blood sugar from going too high or too low.
To prevent lows, always plan and bring a snack to raise your blood sugar if it is needed.
If you experience hypoglycemia during exercise, follow the 15-15 rule:
- Check your blood sugar.
- If your reading is 100 mg/dL or lower, have 15-20 grams of carbohydrate to raise your blood sugar. This may be:
- 4 glucose tablets (4 grams per tablet), or
- 1 glucose gel tube (15 grams per gel tube), or
- 4 ounces (1/2 cup) of juice or regular soda (not diet), or
- 1 tablespoon of sugar or honey
- Check your blood sugar again after 15 minutes. If it is still below 100 mg/dL, have another serving of 15 grams of carbohydrate.
- Repeat these steps every 15 minutes until your blood sugar is at least 100 mg/dL.
If you want to continue your workout, you will usually need to take a break to treat your low blood sugar. Check to make sure your blood sugar has come back up above 100 mg/dl before starting to exercise again.
The time of day you exercise may also have an effect. Exercising in the evening and night might make you more likely to experience on overnight low. Exercising at the end of the day is still feasible, but make sure you adjust your insulin to help prevent a low.
Exercise and hyperglycemia
Blood sugar can also run high during or after exercise, particularly when you do a high-intensity exercise that increases your stress hormone (i.e., glucose-raising hormone) levels.
- If your blood sugar is high before starting exercise, check your blood or urine for ketones. If you test positive for ketones, avoid vigorous activity.
- If you do not have ketones in your blood or urine and you feel well, it should be fine to exercise.
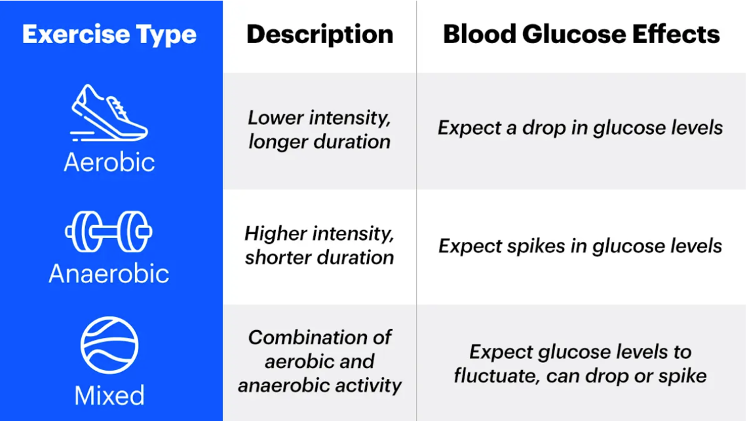
How different types of exercise effect glucose levels:
Aerobic exercise tends to be longer but less intense. It includes activities like running, walking, long-distance swimming, and biking. Typically, these activities will cause blood sugars to drop.
Anaerobic exercise is generally shorter or in spurts but at high intensity. This includes training like sprinting, boxing, ice hockey and weight training. These workouts are great for building muscle and getting stronger. But because of the intensity, these kinds of activities can cause blood glucose levels to spike.
Mixed exercise is a combination of the aerobic and anaerobic activities above. Sports like basketball or soccer fall under this. Because it is a mix of an activity that lowers your blood sugar levels and one that can cause them to spike, it’s easy to see why it’s difficult to manage.
For parents:
The information in this section comes from the American Diabetes Association and the Juvenile Diabetes Research Foundation. For more information regarding exercise and blood glucose, talk with your diabetes healthcare team and check out these resources:
https://www.diabetes.org/healthy-living/fitness/exercise-and-type-1
https://www.diabetes.org/healthy-living/fitness/getting-started-safely/blood-glucose-and-exercise
https://www.jdrf.org/t1d-resources/living-with-t1d/exercise/exercise-impact/
https://www.jdrf.org/t1d-resources/living-with-t1d/exercise/
